Tuberculosis remains one of the world’s deadliest infectious diseases. Currently, the critical challenge has shifted from treatment to detection.
A growing body of evidence shows that a significant share of people with TB do not present symptoms but remain infectious. For health systems already under pressure, this raises a critical question: how do you find patients who don’t know they’re sick?
A Persistent Global Burden
According to recent global estimates, more than 10 million people develop tuberculosis each year, and over 1.3 million die from the disease annually1. While global efforts have improved access to treatment, detection gaps remain a major barrier to control.
In sub-Saharan Africa, the burden is particularly high. Many countries continue to face:
- Limited diagnostic infrastructure
- Delays in laboratory confirmation
- Uneven access to advanced imaging and molecular testing
These challenges contribute to ongoing transmission, often driven by patients who are not diagnosed early.
The Limits of Symptom-Based Screening
For decades, TB detection strategies have relied heavily on symptom screening, typically focusing on patients presenting with a persistent cough, fever, or weight loss.
However, recent findings suggest this approach may be missing a substantial number of cases.
“Symptom-based screening misses a big group,” says Dr. Stephen John, Director of Planning, Research and Statistics at the Adamawa State Ministry of Health in Nigeria.
“From prevalence surveys in Nigeria, close to 40–45% of people with TB are asymptomatic, and they are bacteriologically positive. They are spreading the illness.”
This means that nearly half of TB cases in some settings may not be captured through traditional screening methods alone.
Imaging as a Triage Tool

To address this gap, some TB programs are incorporating chest X-ray earlier in the diagnostic pathway.
Unlike symptom screening, imaging can reveal structural changes in the lungs, even in patients who do not report symptoms.
“With this equipment, you are able to triage and pick out people that are really presumptive,” Dr. John explains.
“Even those that are asymptomatic, you can begin to see features on the lung image that suggest TB.”
Patients identified through imaging can then be referred for confirmatory testing, such as molecular diagnostics (e.g., GeneXpert), helping to prioritize limited laboratory resources.
A Practical Role in Resource-Constrained Settings

At Village of Hope Hospital in Kenya, chest X-ray plays a key role in how suspected TB cases are managed, both for triage and early treatment decisions.
Radiographer Brandy Jeruto describes the day-to-day reality: “When a patient comes in with symptoms like cough or weight loss, we request an X-ray. If the X-ray is suggestive of TB, the patient is started on medication while we await lab confirmation.”
GeneXpert testing is not available on-site, requiring samples to be sent to external facilities, a delay that can have public health implications. “If we did not have the X-ray, we would send the patient home to wait,” Jeruto explains. “They could interact with others, and transmission could continue.”
For clinicians, imaging helps bridge that gap, guiding early decisions when time matters most.
Clinical Officer Joy Juma says the impact has been measurable at the facility level: “Since we acquired the X-ray system, we have significantly improved our ability to diagnose tuberculosis early and accurately. We have diagnosed and treated over 50 patients with TB, all with positive outcomes.”
Beyond individual cases, the availability of imaging has also expanded access to care in the surrounding community. “More people are now able to access essential diagnostic services close to home,” Juma adds. “It has strengthened our services and improved the quality of care we provide.”
In this setting, X-ray is not only supporting diagnosis, it is helping accelerate treatment, reduce delays, and limit ongoing transmission.
Expanding the Role of X-ray
Recent developments in X-ray technology are also influencing how imaging is used in TB programs.
Systems that provide additional image information — such as separating soft tissue and bone structures — are being introduced in some regions to support more detailed interpretation of chest images.
KA Imaging’s Reveal 35C detector, for example, is currently installed in both Nigeria and Kenya as part of local imaging initiatives. These systems aim to provide multiple image outputs from a single acquisition, which may support clinicians in identifying subtle lung abnormalities.
While such technologies are still being evaluated in different settings, they reflect a broader trend: using imaging not just for diagnosis, but as an early triage tool.
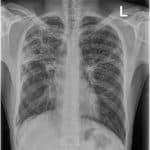
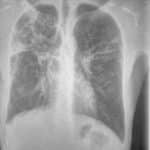
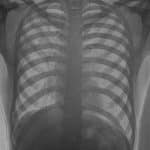
A 22-year-old male presented with a one-month history of dry cough and chest pain. Chest X-ray findings were suggestive of tuberculosis, later confirmed by GeneXpert testing.
Early Impact in Local Programs
In Nigeria, integrating imaging into TB workflows has coincided with improvements in case detection.
“If you look at the data coming out of Kaduna in the past few years, there has been a remarkable improvement in the number of people diagnosed and treated,” says Dr. John.
Although multiple factors contribute to these outcomes, strengthening front-line detection — particularly for asymptomatic patients — is considered a key component.
Rethinking Detection Pathways
Public health experts increasingly point to the need for a more integrated approach to TB detection.
Rather than relying solely on symptoms, a combined model may include:
- Imaging for early triage
- Targeted molecular testing for confirmation
- Faster linkage to treatment
This approach may help reduce missed cases, improve efficiency, and limit transmission.
Looking Ahead
As countries work toward global TB reduction targets, improving early detection remains a priority.
“If we want to reduce the burden of TB globally, we need to identify patients earlier in the disease pathway,” says Amol Karnick, CEO of KA Imaging.
“Strengthening front-line tools like X-ray, and improving the amount of clinical information available from each exam, can support more effective screening and better use of existing diagnostic infrastructure.”
World TB Day: Closing the Detection Gap
This World TB Day highlights a central challenge in TB control: the gap between those who have the disease and those who are diagnosed.
In many parts of the world, that gap is shaped not only by access to treatment, but by the ability to detect TB early, especially in patients without symptoms.
As new approaches and technologies are introduced, the focus remains the same:
finding more patients, sooner, and connecting them to care.
Because in the effort to end TB, detection is where progress begins.
References:
1 https://www.who.int/publications/i/item/9789240116924 Top of Form